Let’s be honest, January was a bad month for healthcare news coming out of China.
For starters, at the end of December, a Chinese court sentenced He Jiankui to three years in prison for operating an illegal medical practice, which includes using a fake ethical review certificate and misleading participants about a study’s risks, and also violating an ethics guidance from 2003 that barred the reproductive use of research embryos.
You may remember Dr Jiankui as the individual who made the world’s first genetically edited babies by recruiting couples in which the man was HIV positive but the woman was not, as part of an effort to create embryos with a genetic mutation that made the couples’ offspring protected from the virus.
Esteemed bioethicists and scholars, such as Josephine Johnston from the Hastings Center that produces books, articles and other publications on ethical questions in medicine, science and technology that help inform policy, practice and public understanding, as well as Robin Lovell-Badge, a stem cell biologist at the Francis Crick Institute, have both acknowledged that He Jiankui’s work straddled a line that might have got them in hot water in both the US and the UK.
In fact, Lovell-Badge said in a statement distributed by the United Kingdom’s Science Media Centre that “both prison and a fine would have been the likely penalties if someone had done what [He Jiankui] did in the UK”.
And then, in early January, China informed the world about a deadly new coronavirus that has been causing severe respiratory illness and death among its citizens.
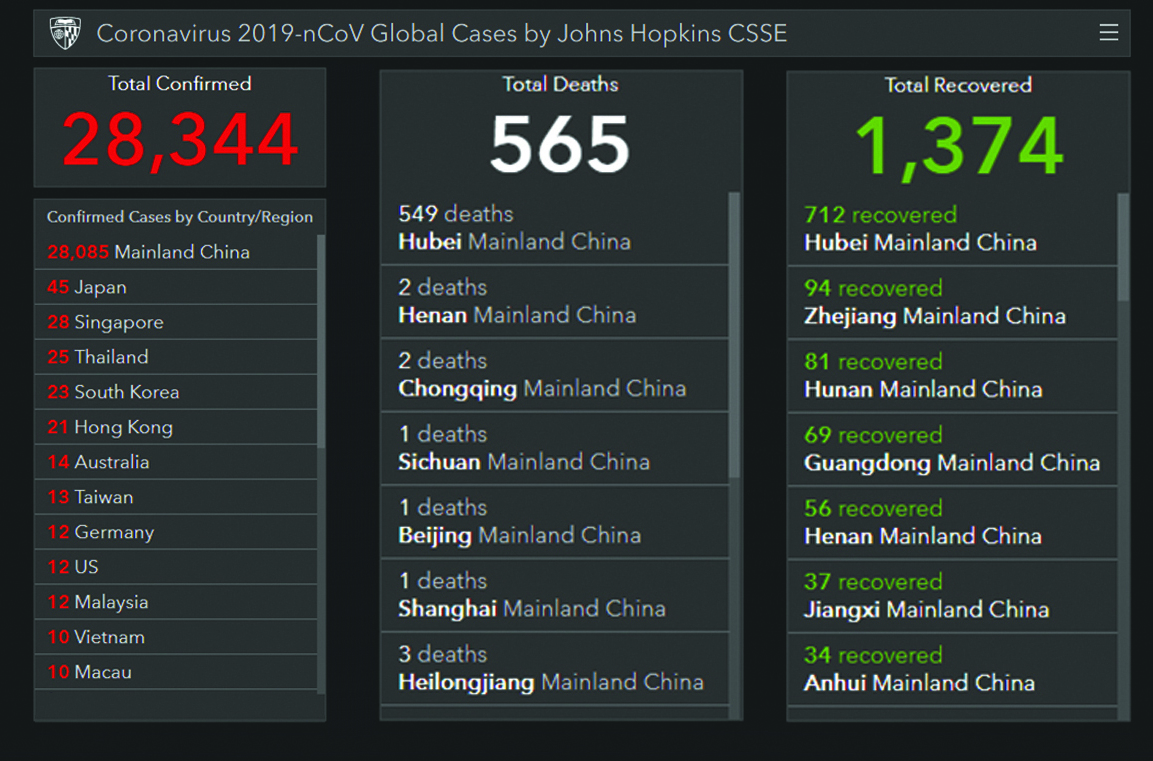
As of 6 February, in China there were over 28,000 confirmed cases and 565 people have died there; in addition there were more than 220 confirmed cases outside China and there has been one death in the Philippines.
On 26 January, the New York Times wrote: ‘The outbreak has drawn fresh attention to China’s animal markets, where the sale of exotic wildlife has been linked to epidemiological risks. The Wuhan virus is believed to have spread from one such market in the city. The SARS outbreak nearly two decades ago was also traced back to the wildlife trade.’
These two scenarios highlight an important aspect of public health and health policy: complex decisions that require almost real-time response are only as good as the information upon which those decisions are based.
In the case of He Jiankui, many countries have policies and laws in place against germline gene editing. But because the court proceedings, documentation and testimony in this case have not been made public, it is impossible to know the details surrounding the events that may have facilitated this ‘rogue scientist’s’ behaviour.
And because we don’t have those details, implementing new health policy to prevent recurrences of this situation remains difficult. Not impossible, but difficult. Some will argue that US and UK laws are expansive enough and the penalties imposing enough on their own merits that we need not fret about a single scientist’s actions in a universally agreed upon opaque scientific ecosystem.
Others will argue that the scientific community’s overwhelmingly negative response and outrage will discourage this from happening again. I disagree.
And in the coronavirus situation, the same New York Times article went on to say: ‘Conclusive evidence about how this outbreak started is lacking. Although officials in Wuhan first traced it to a seafood market, some who have fallen ill never visited the market.
‘Researchers have also offered disparate explanations about which animals may have transmitted the virus to humans. China’s record doesn’t help. During the SARS epidemic in 2002 and 2003, officials covered up the extent of the crisis, delaying the response. The Chinese government has promised far more transparency this time, and the World Health Organization (WHO) has praised its cooperation with scientists.’
I’m sure we all feel better that a non-partisan agency like the WHO has authenticated the cooperation of the Chinese scientific community in 2020 but the issue is far more complex.
We need to understand the larger social and cultural issues that may be driving the underlying causes of these deadly illnesses. And in order to do that, the Chinese government’s openness to the rest of the world’s questions and, ultimately, its willingness to revise public policy to reflect a greater harmonisation for global public health will be put to the test.
This is not a ‘China’ issue. It’s a transparency issue. Whether it’s the reporting of a measles outbreak in America or the promulgation of information on Ebola cases in West Africa, we are all responsible because the world needs more transparency.